Health
Osteoporosis is a silent disease. Check your bone heath regularly, writes Shivani Arora.
Osteoporosis is becoming an increasingly common metabolic bone disorder in silvers, more so in women. It is important to understand this disorder and take care of one’s bones because the downside of this disease is that it can easily lead to fractures. We address common concerns regarding osteoporosis by speaking to Dr Ambrish Mithal, chairman, Department of Endocrinology, Medanta The Medicity; chief advisor of the ISBMR (Indian Society for Bone and Mineral Research); and board member of the International Osteoporosis Foundation.
What is osteoporosis?
‘Osteo’ means ‘bone’ while ‘porosis’ means ‘porous’. Osteoporosis therefore means ‘porous bones’. This is a silent condition, where bones become brittle and break with minor or sometimes even no injury. It is a result of reduction in bone density as well as deterioration in bone quality over years. As we grow, our skeleton accumulates bone mass; we attain our peak bone mass by about 20 years of age. Thereafter, we maintain it for about 15 years. Subsequently, we lose bone mass throughout life, albeit at a slow rate. This bone loss is accelerated around menopause in women for a few years. It happens silently, without warning, till it reaches a critical level and a fracture occurs.
How does it affect the elderly, more so women? Are men also prone to it?
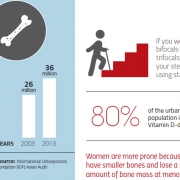
Women are more prone because they have smaller bones and lose a significant amount of bone mass at menopause. Oestrogen is a key protector of the skeleton and prevents bone loss. Once oestrogen declines at menopause, calcium leaks out from the bones, leading to osteoporosis. Men are also prone, although less than women. At the age of 50, the lifetime risk of fracture is one in three for women and one in five for men.
Does the condition show any initial symptoms?
There are no symptoms of bone loss. Symptoms occur only when a bone fractures. Common fractures are those of the wrist, spine and hip. Hip fractures are most serious and can even be fatal sometimes. Spine fractures can occur with minimal or no symptoms—maybe just a backache that may be dismissed as a ‘muscle spasm’, although at times they can occur with excruciating pain necessitating surgical intervention.
How is osteoporosis diagnosed?
The diagnosis is made by measuring bone density using Dual Energy X-Ray Absorptiometry (DXA). This is a non-invasive test that takes only a few minutes. It provides the ‘T scores’ of the patient that help diagnose whether the patient has osteoporosis. The National Osteoporosis Foundation of the US recommends this test routinely for women over 65 and men over 70. It should be done earlier if there is reason for accelerated bone loss like use of corticosteroid medication or other conditions that cause bone loss. It is also very useful to do a lateral spine X-ray to pick up unidentified silent spine fractures.
What is the mode of treatment for osteoporosis?
The fundamentals of prevention and treatment of osteoporosis are nutrition and exercise. Adequate calcium and protein in the diet is a must. The chief source of calcium is milk and milk products. Those who are diagnosed with osteoporosis should take calcium pills. An intake of at least 1,000 mg calcium daily is advisable.
The other critical factor is the Vitamin D status. Vitamin D is essential to absorb calcium; without Vitamin D, the calcium in our diet is not absorbed and thus does not reach our bones. Vitamin D deficiency is widespread in India owing to our tendency to avoid the sun, and the fact that our skin pigment reduces the efficiency of Vitamin D synthesis. Also, food in India is generally not fortified with Vitamin D whereas in most Western countries, milk and milk products are. It is mandatory to correct Vitamin D deficiency to get optimum benefit from osteoporosis medication. This usually means about 2,000 IU/day Vitamin D for Indians.
Some drugs can reduce bone resorption, like bisphosphonates. Alendronate and Risedronate are given weekly; Ibandronate monthly. The most popular and potent bisphosphonate these days is Zoledronic Acid, given as an intravenous infusion once a year. For bone formation, the preferred drug is PTH (Teriparatide) which is used as a daily ‘pen’ selfinjection for 18-24 months. These drugs can reduce risk of fracture by 40-50 per cent.
With the widespread deficiency of Vitamin D among Indians, is osteoporosis a major cause of worry for the elderly?
Yes. With estimates showing that about 80 per cent of the urban Indian population is Vitamin D-deficient and hip fractures occur about a decade earlier than in Western countries, osteoporosis is certainly a major concern for our ageing population. In the 2009 International Osteoporosis Foundation (IOF) Asian Audit, expert groups estimated that the number of patients suffering from osteoporosis in India was 26 million in 2003, with projections indicating 36 million patients by 2013. In 2013, sources estimated that 50 million people in India are either osteoporotic (T-score lower than -2.5) or have low bone mass (T-score between -1.0 and -2.5).
FALL PREVENTION TIPS
Regular physical activity, including exercises for balance, strength and posture
Consider attending a ‘fall prevention’ or ‘falls and balance’ programme
Use a walking aid, if needed, for balance
Talk to your doctor if you suffer from dizziness or feel unsteady
Wear shoes with good foot support—broad heel, non-slip soles
Get your eyes tested annually by an optometrist
Wear sunglasses outside to minimise glare and squinting
Maintain a healthy diet that includes fresh fruit and vegetables and calcium-rich foods
Review all medications with your doctor on a regular basis
ELIMINATE HOUSEHOLD HAZARDS
Floors: Try to keep furniture in its usual place, remove cords, loose wires and clutter. Ensure rugs and mats are securely fixed and smooth
Bathrooms: Install handrails and a non-skid mat or tape
Kitchen: Mop up spills near the sink and stove immediately. Install non-skid rubber mats. Keep kitchen items used regularly at a comfortable, easy-to-reach height to avoid reaching and bending
Lighting: Keep staircases, entrances and halls well lit. If you get up during the night, turn on lights; use automatic lights and glow tapes
Photo: iStock Featured in Harmony — Celebrate Age Magazine July 2016
you may also like to read
-
Hot tea!
If you enjoy sipping on that steaming hot cup of tea, think twice. New research establishes a link between drinking….
-
Weight and watch
If you have stayed away from lifting weights at the gym, thinking it might not be a good idea for….
-
Toothy truth
Research has established a clear association between cognitive function and tooth loss when cognitive function score was categorised into quintiles…..
-
PRODUCT OF THE MONTH
Automatic Blood Pressure Monitor Measure your blood pressure and pulse rate with no fuss Hypertension, or high blood pressure, could….