Health

Endoscopic spinal surgery is a safe surgical option for treating lumbar spinal stenosis (back pain) in silvers. Dr Abhijit Y Pawar, consultant spine surgeon at Mumbai’s Kokilaben Dhirubhai Ambani Hospital, elaborates upon this effective alternative to open-back surgery and discusses why surgeons are gradually adopting it
More than 80 per cent of elderly Indians between the ages of 60 and 80 years experience crippling back and leg pain. Of these individuals, 25 per cent might have osteoarthritis, 35 per cent have mild spinal stenosis (narrowing) and 19 per cent have significant symptomatic stenosis of the spinal canal. It mainly appears with age, but the arthritis-like condition may also appear in younger individuals. Back pain takes a toll not only on patients but their family and friends. Many a time, patients find that along with their back health, their relationships slowly deteriorate. It is, therefore, important to treat it at the earliest.
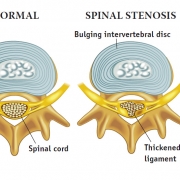
What is spinal stenosis?
Lumbar spinal stenosis occurs in the spinal column where the spinal cord, nerve roots and vertebrae are located. Over time, the spinal canal may become constricted or narrowed. This is characterised by ‘neurogenic claudication’, which is back pain, leg pain, numbness and tingling made worse by sitting, bending and arching back. It is exacerbated by walking and spinal extension. Some elderly patients also have spinal stenosis owing to a slipped intervertebral disc. This is commonly called sciatica. Sciatica is often associated with leg numbness or paresthesias and weakness in the legs.
What is endoscopic spinal surgery?
When it comes to open-back surgery, a patient’s age is an important consideration. Older surgical patients are more prone to serious medical conditions such as diabetes and heart disease, precluding them from undergoing open-back surgery. Also, older patients who undergo an invasive surgical procedure are more likely to suffer from an infection, life-threatening complication, or a return visit to the hospital within 30 days post-surgery. Therefore, endoscopic spinal surgery is the need of the hour.
The right candidate for endoscopic spine surgery is any elderly patient who has persistent neurogenic claudication or sciatica and has no relief of symptoms after four to six weeks of conservative management, including rest and physical therapy. If patients have a medical problem like diabetes or heart disease putting them at risk during general anaesthesia, endoscopic spine surgery, also called endoscopic discectomy, can be done under local anaesthesia.
Endoscopic discectomy and the technique
Endoscopic discectomy is a minimally invasive spinal surgery technique that utilises an endoscope to treat herniated, protruded, extruded or degenerative discs that are a contributing factor to leg and back pain. The endoscope allows the surgeon to use a keyhole incision to access the herniated disc. Muscle and tissue are dilated rather than being cut when accessing the disc. This leads to less tissue destruction, less postoperative pain, quicker recovery time, earlier rehabilitation and avoidance of general anaesthesia. The excellent visualisation via the endoscope permits the surgeon to selectively remove a portion of the herniated nucleus pulposus (the inner core of the vertebral disc) contributing to the patients’ leg and back pain.
This minimally invasive procedure is performed through a small tubular device under local or general anaesthesia, allowing the patient to leave the hospital the same day. After the disc protrusion is confirmed, a guide wire is inserted to the affected disc under fluoroscope guidance. An obturator tube is passed over the guide wire to push apart the tissue down to the disc and move the nerve root out of the way. The working sleeve, through which the surgery will be performed, is slid over the dilating tube. The guide wire and dilator are then removed. The surgeon uses instruments to remove the degenerative and extruded portions of the disc nucleus. As only enough of the disc is removed to reduce pressure inside the disc, the spine remains stable. The foramen (opening, hole or passage) and nerves are inspected to confirm successful decompression. The instruments and sleeve are removed. No muscles or bone are cut during the procedure, so recovery is fast and scarring is minimised. The patient may only need a day of bed rest after the procedure and physical therapy.
The advantages
- Endoscopic spine surgery can be done under local anaesthesia and sedation.
- It involves a one-day hospital stay.
- As there’s no general anaesthesia, it is safe for patients with problems like diabetes, heart disease and those of advanced age.
- There is predictable relief of back and leg pain.
- No loss of blood.
- No risk of infection.
- Minimal need for antibiotics.
- Tissue is spared and there is less postoperative scar tissue formation.
- There is quicker healing with less rehabilitation and rapid return to activities.
- This is a safe approach without damage to the nerve root, ganglion or dura.
In conclusion
Although age is a consideration for most surgical procedures, it is a lesser determinant for endoscopic surgery. Rather than performing a laminectomy to completely remove the lamina, endoscopic procedures perform a laminotomy or partial removal of the lamina, which preserves more of the lamina and decreases the odds of spinal instability in future years. According to peer-reviewed journal articles, science is on the side of minimally invasive spine surgery, touting it as a safe and effective alternative to open-back surgery for older adults. Many surgeons and medical practices are slowly migrating toward this technique. Indeed, the endoscopic technique is a permanent solution for many patients, allowing them to preserve mobility and return to their routines and favourite activities. Older patients with back problems can thus benefit greatly from endoscopic spine surgery.
Photos: 123RF.com Featured in Harmony — Celebrate Age Magazine May 2017
you may also like to read
-
Hot tea!
If you enjoy sipping on that steaming hot cup of tea, think twice. New research establishes a link between drinking….
-
Weight and watch
If you have stayed away from lifting weights at the gym, thinking it might not be a good idea for….
-
Toothy truth
Research has established a clear association between cognitive function and tooth loss when cognitive function score was categorised into quintiles…..
-
PRODUCT OF THE MONTH
Automatic Blood Pressure Monitor Measure your blood pressure and pulse rate with no fuss Hypertension, or high blood pressure, could….